When Blood Types Don’t Match: Why Rapid Compatibility Testing Saves Lives
When blood types don’t match, the consequences can be life-threatening. A transfusion with incompatible blood can trigger severe immune reactions that damage red blood cells, leading to complications such as organ failure or shock. Rapid compatibility testing helps prevent these risks by quickly identifying safe donor–recipient matches, ensuring that patients receive the right blood in critical situations where every second matters.
2/18/20262 min read
A Race Against Time in the Emergency Room
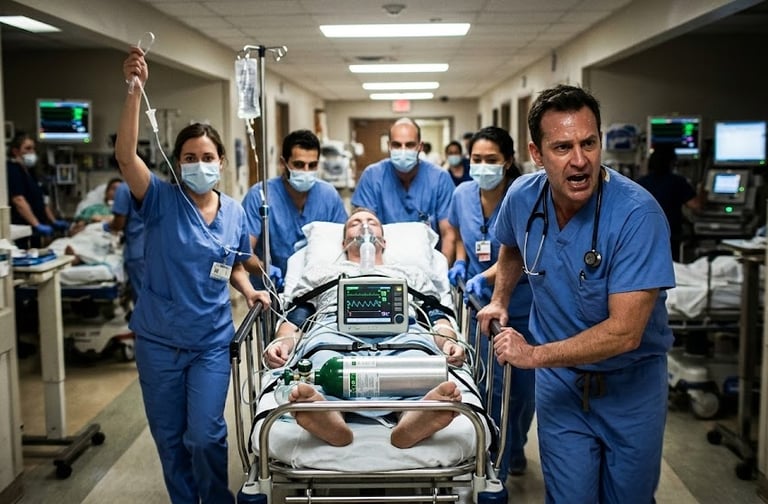
In a busy emergency room, seconds can decide the difference between life and death.
A patient is rushed in after a severe accident, losing blood rapidly. Doctors move quickly—oxygen, IV lines, monitors—but one critical question must be answered first:
What blood can we safely give this patient?
Blood transfusion is one of medicine’s most powerful life-saving tools. But behind every transfusion lies an important reality:
Not all blood is the same.
When incompatible blood enters the body, the consequences can be severe.
Why Blood Types Matter
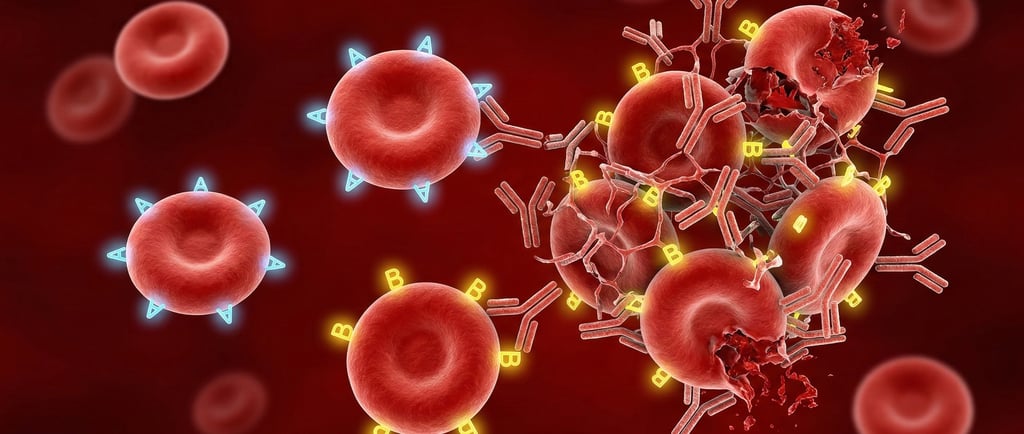
Each person’s red blood cells carry tiny molecular markers called antigens.
These markers determine a person’s blood group.
The main blood group systems include:
ABO system
Type A
Type B
Type AB
Type O
Rh factor
Rh-positive
Rh-negative
While these labels may appear simple, the immune system treats them very seriously.
When foreign blood enters the body, the immune system recognizes unfamiliar antigens and responds immediately.
What Happens When Blood Types Don’t Match
If incompatible blood is transfused, the body can trigger a hemolytic transfusion reaction.
During this reaction:
Antibodies attack the donor red blood cells
Cells may clump together (agglutination)
Red blood cells may break apart (hemolysis)
This reaction can cause serious complications, including:
Fever and chills
Severe inflammation
Kidney damage
Breathing difficulty
Dangerous drops in blood pressure
Life-threatening shock
What was intended to save a life can quickly become another medical emergency.
The Critical Role of Compatibility Testing
Because of these risks, doctors never rely on guesswork before giving blood.
Before a transfusion, laboratories perform several safety checks.
Standard compatibility testing includes:
1. Blood Typing
Determines the patient’s ABO group
Identifies the Rh factor
2. Antibody Screening
Detects unusual antibodies in the patient’s blood
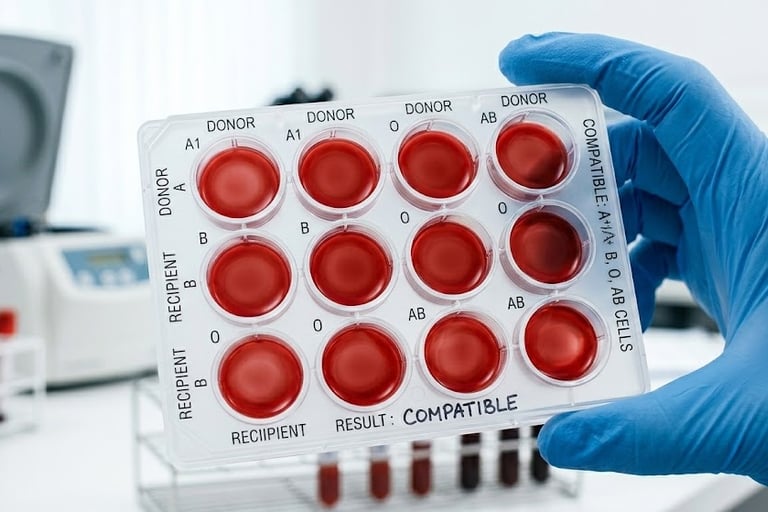
3. Crossmatching
Tests donor blood directly against the patient’s plasma
Confirms that the two are compatible
These steps act as a critical safety checkpoint before any transfusion.
“The right blood to the right patient at the right time is the foundation of safe transfusion practice.”
— Transfusion Medicine Principle
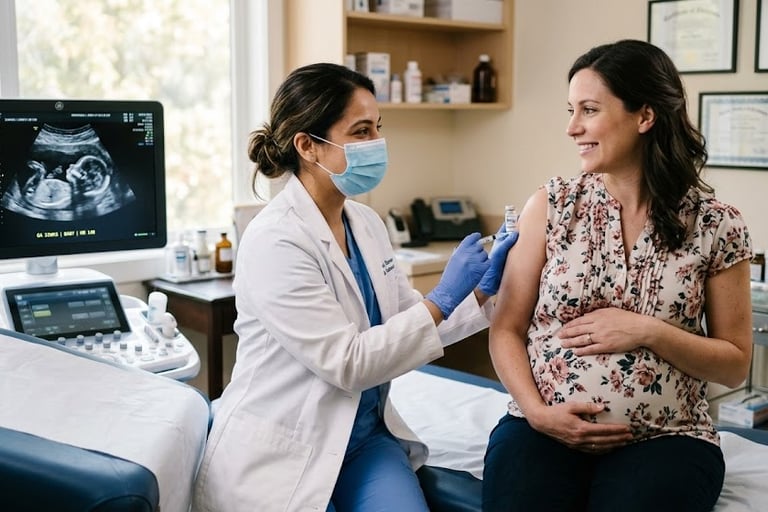
Why Blood Compatibility Matters in Pregnancy
Blood compatibility is also essential during pregnancy.
A complication can occur if:
The mother is Rh-negative
The baby is Rh-positive
In this situation, the mother’s immune system may produce antibodies against the baby’s red blood cells.
This condition is called:
Rh Incompatibility
It can lead to Hemolytic Disease of the Newborn (HDN), which may cause:
Severe anemia in the baby
Jaundice
Organ damage
Fortunately, modern prenatal care prevents most cases.
Preventive measures include:
Routine blood typing during pregnancy
Antibody screening
Rh immunoglobulin injections
These treatments protect both the baby and future pregnancies.
The Challenge of Time in Medical Emergencies
In trauma situations, time becomes a critical factor.
A patient with severe blood loss cannot wait hours for laboratory testing.
Without rapid transfusion:
Oxygen delivery drops
Organs begin to fail
Survival chances decrease rapidly
This is where rapid compatibility testing becomes vital.
How Rapid Testing Saves Lives
Modern medical technology now allows compatibility testing to be performed within minutes.
Advanced tools include:
Automated blood analyzers
Point-of-care diagnostic devices
Portable blood typing systems
These technologies allow doctors to:
Identify safe blood types quickly
Reduce transfusion delays
Provide life-saving treatment during trauma
Speed and accuracy must work together.
The Silent Guardian of Safe Transfusions
Blood transfusions may appear routine, but every successful procedure depends on careful verification.
Rapid compatibility testing works quietly behind the scenes to ensure:
The right blood
Goes to the right patient
At the right time
Because when blood types don’t match, the body reacts immediately.
And in those critical moments, knowing the answer quickly can mean the difference between danger—and survival.